Impact of Climate Change on Antibiotic Resistance
Each year, it is estimated that there are over 2 million antibiotic-resistant infections in the United States alone. Of these, approximately 23,000 infections result in fatalities [1]. A major driving force behind the rise of antibiotic-resistant bacteria is the increasing consumption and overuse of antibiotics [7], and it is estimated that by 2050, the number of deaths due to antibiotic resistance could reach 10 million annually [4]. However, these projections often overlook an important factor: climate change. A recent study has found that rising temperatures and increasing population density are significant contributors to the development of antibiotic resistance, representing an escalating threat to global public health.
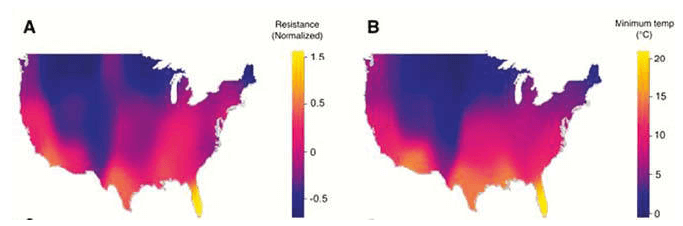
This recent study, published in Nature, demonstrates a direct correlation between antibiotic resistance, population density, and the accelerating pace of global warming [6]. The researchers examined how resistance in three common bacterial pathogens: Escherichia coli, Klebsiella pneumoniae, and Staphylococcus aureus, changes in response to shifts in temperature and population density. They found a clear association between increased local temperatures and higher rates of antibiotic resistance (Fig. 1).
Figure 1: Antibiotic resistance increases with increasing temperature. (A) A heatmap of mean normalized antibiotic resistance for E. coli for all antibiotics across the USA. (B) A heatmap of 30-year average minimum temperature (oC) across the USA [5].
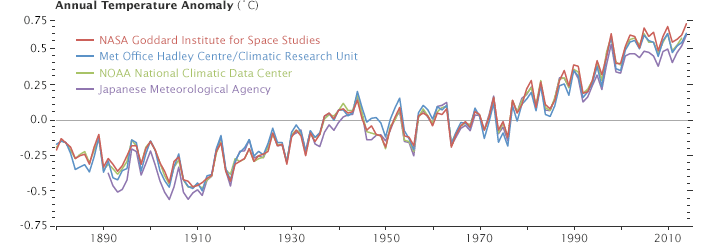
Multiple studies and climate surveys have shown that global average temperatures have steadily increased over the past century. According to data from NASA and other international agencies, annual average temperatures are on a continuous upward trajectory (Fig. 2). If this trend persists, the increasing temperatures may also contribute to the acceleration of antibiotic resistance.
Figure 2: Data collected by NASA and NOAA (United States), Japanese Meteorological Agency (Japan), and the Met Office Hadley Center (United Kingdom) from 1880 to 2014 show similar trends in global temperature. All four recorded a rapid warming trend in the last decade [8].
One biological explanation for this phenomenon involves enzyme activity. Many enzymes exhibit a 50% to 100% increase in activity when the temperature rises by just 10°C [3]. In bacteria, increased enzyme activity leads to faster replication rates. As the planet warms, these elevated enzymatic activities promote quicker bacterial growth. Since antibiotic resistance genes propagate during bacterial replication, mutation rates and resistance spread more rapidly under higher temperatures.
In their analysis of data from facilities across the U.S., the researchers found that a 10°C increase in minimum temperature corresponded to a rise in resistance of 4.2%, 2.2%, and 2.7% in E. coli, K. pneumoniae, and S. aureus, respectively [6]. Minimum temperature was selected over average temperature because it better reflects sustained bacterial growth conditions, with population density and antibiotic prescription rate controlled as variables. The study also observed that antibiotic resistance prevalence is typically higher in southern U.S. states compared to northern ones, likely due to regional temperature differences.
The research team also investigated how population density affects resistance rates. They discovered that increasing the population density by 10,000 people per square mile led to a 3% to 6% increase in resistance among the three bacterial strains [2]. As urban populations continue to grow, this factor will likely compound the challenges of controlling antibiotic-resistant infections.
Developing innovative strategies to combat drug-resistant bacterial infections is becoming increasingly urgent for the medical and scientific communities. At Emery Pharma, we are committed to supporting this fight. We maintain an extensive library of multi-drug resistant bacterial strains, each with unique, well-characterized resistance mechanisms. Our microbiology and antibiotic testing services help evaluate the efficacy of novel drug candidates, identify mechanisms of action, assess activity against biofilms, and more. For more information or to consult with our scientific team, contact us online or call us at +1 (510) 899-8814!
About the author
Originally authored by Benjamin Linetsky. This article was reviewed and updated on July 11, 2025 by Dr. Janet Liu, current Director of Biology.
References
- Be Antibiotics Aware: Smart Use, Best Care. (2018, November 09). Retrieved from http://www.cdc.gov/features/antibioticuse/index.html
- Brouillette, M. (2018, May 21). A Warming Climate May Produce More Drug-Resistant Infections. Retrieved from https://www.scientificamerican.com/article/a-warming-climate-may-produce-more-drug-resistant-infections/
- Introduction to Enzymes. (n.d.). Retrieved from http://www.worthington-biochem.com/introbiochem/tempeffects.html
- Kraker, M. E., Stewardson, A. J., & Harbarth, S. (2016). Will 10 Million People Die a Year due to Antimicrobial Resistance by 2050? PLOS Medicine,13(11). doi:10.1371/journal.pmed.1002184
- Macfadden, D., Mcgough, S., Fisman, D., Santillana, M., & Brownstein, J. (2017). Antibiotic Resistance Increases with Local Temperature. Open Forum Infectious Diseases. doi:10.1093/ofid/ofx163.327
- MacFadden, D. R., McGough, S. F., Fisman, D., Santillana, M., & Brownstein, J. S. (2018, May 21). Antibiotic resistance increases with local temperature. Retrieved from https://www.nature.com/articles/s41558-018-0161-6
- Ventola, C. L. (2015). The Antibiotic Resistance Crisis Part 1: Causes and Threats. Journal for Managed Care and Hospital Formulary Management,277-283. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4378521/.
- World of Change: Global Temperatures. (n.d.). Retrieved from https://earthobservatory.nasa.gov/WorldOfChange/decadaltemp.php