Testing of Toxins and Toxin Inactivating Compounds

Figure 1. Several of the toxins used in prior Emery Pharma projects. From left to right: α-hemolysin toxin from Staphylococcus aureus, enterotoxin type B from Staphylococcus aureus, and streptolysin O from Streptococcus pyogenes.
Toxins are naturally occurring poisonous substances produced by living cells. These biological toxins, also known as biotoxins, differ from synthetic toxicants. Biotoxins are found in a wide range of organisms: from honey bees that release apitoxin when they sting, to venomous snakes with protein-based toxins. Many single-celled organisms, including bacteria and yeast, also produce toxins. Despite their toxicity, some biotoxins have pharmaceutical applications. For example, warfarin—a widely prescribed anticoagulant—was synthetically derived from dicoumarol, a naturally occurring fungal toxin initially used as a rat poison [1].
 |
|
| Figure 2. Amanita phalloides, commonly referred to as “deathcap” mushrooms, contain many different toxins and account for the majority of deaths associated with mushroom poisoning. |
Microbial toxins are commonly classified into two types: endotoxins and exotoxins. Endotoxins are lipopolysaccharides embedded in the outer membrane of Gram-negative bacteria, released when the cell lyses. In contrast, exotoxins are proteins secreted by both Gram-positive and Gram-negative bacteria during growth. One of the most dangerous toxins known is botulinum toxin—an exotoxin from Clostridium botulinum—which is lethal in doses as small as several nanograms per kilogram. Table 1 summarizes some of the key differences between endotoxins and exotoxins.
Table 1: Endotoxins vs. Exotoxins
| Endotoxin | Exotoxin | |
| Gram-positive or negative | Gram-negative | Both |
| Heat Stable | Yes | No |
| Structure | Lipopolysaccharide | Protein |
| Location | Cell Wall | Varies |
| Release | Upon Lysis | During Growth |
| Relative Toxicity | Low | High |
| Specificity | Low | High |
 |
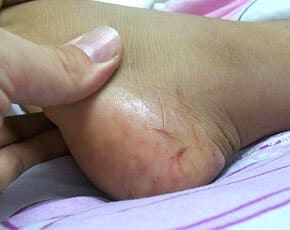 |
| Figure 3. A patient infected with Yersinia pestis, the bacteria responsible for the bubonic plague. Yersinia murine toxin (Ymt) and endotoxins play crucial roles in the disease state. | Figure 4. A rattlesnake bite on a foot. The inflammation observed is a result of protein toxins in rattlesnake venom. |
Different microorganisms produce specific toxins that contribute to disease pathology. These toxins can directly damage host tissues and modulate immune responses. For example, Escherichia coli produces Shiga toxins, which inhibit protein synthesis by hydrolyzing RNA. In severe cases, Shiga toxin exposure can lead to hemolytic-uremic syndrome, marked by red blood cell destruction and kidney failure.
Staphylococcus aureus produces a wide range of toxins including superantigens like enterotoxins A and B, which trigger massive immune responses and can result in toxic shock syndrome. It also produces exfoliative toxins, responsible for staphylococcal scalded skin syndrome (bullous impetigo), primarily affecting children. Other S. aureus toxins include α-, β-, and δ-toxins, with α-hemolysin notably contributing to lung inflammation in pneumonia.
Streptococcus pyogenes is another pathogen that secretes multiple toxins, including Streptolysin O and S and Streptococcal pyrogenic exotoxins A and C (SpecA and SpecC). These toxins are associated with diseases such as scarlet fever, streptococcal toxic shock syndrome, and necrotizing fasciitis (flesh-eating disease). This aggressive condition involves rapid tissue destruction due to toxin release and can lead to septic shock, limb amputation, or death [2].
 |
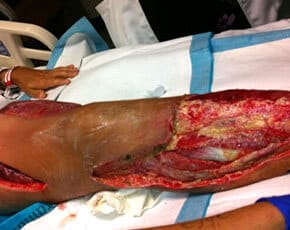 |
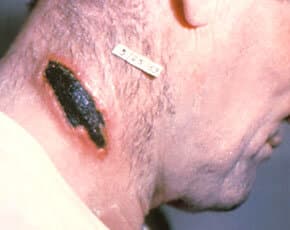
| Figure 5. A lesion and cutaneous reaction caused by anthrax toxin, a protein exotoxin released from Bacillus anthracis. Cutaneous anthrax, or Hide-porter’s disease, is less lethal than pulmonary anthrax. | Figure 6. A patient with necrotizing fasciitis, or flesh-eating bacteria. Tissue damage to the leg is a result of bacterial exotoxins. |
Even within the same bacterial species, different strains may produce different toxins. For example, although S. aureus is commonly found on healthy skin, certain toxin-producing strains are highly pathogenic. This variation underscores the importance of identifying and neutralizing toxins during infection treatment. Toxins can delay wound healing, making the evaluation of toxin-inactivating compounds a critical component in therapeutic development.
One effective approach to measure toxin activity is cytotoxicity testing using cultured cells. A common metric used is the CT50, or the concentration that kills 50% of the cells. To assess the efficacy of a toxin-inactivating compound, the toxin is first incubated with various concentrations of the compound. After incubation, the mixture is applied to cells, which are later analyzed for viability. The EC50, or half-maximal effective concentration, helps determine how well the compound neutralizes the toxin. Emery Pharma has extensive experience conducting such studies using a wide range of cell lines and methodologies .
Emery Pharma offers comprehensive services to evaluate both toxin activity and the effectiveness of toxin-inactivating compounds. We also support custom study design for a variety of toxin-related applications. For expert consultation or to learn more about our capabilities, please contact Emery Pharma today!
References:
1) Smitt CK, Meysick KC, O’Brien AD. Bacterial Toxins: Friends or Foes? Emerging Infectious Diseases. 1999;5(2):224-34.
2) Wong C, Kurup A, Tan KC. Group B Streptococcus necrotizing fasciitis: an emerging disease? European Journal of Clinical Microbiology. 2004;23:573-575.
