Infection by Site
Choosing the Right Bacteria and Antibiotic in Novel Anti-infective Discovery
The development of new drugs to treat infectious disease requires a great understanding of bacteria and their primary sites of infection. Antibiotic selection should be characterized by two things: 1) Spectrum of activity, and 2) Ability to penetrate the site of infection.
As widely distributed as they are, many microbes are highly adapted to a specific environment due to metabolic and/or temperature requirements for growth and replication. For example, obligate anaerobic bacteria cannot grow in the presence of atmospheric oxygen, as they lack the metabolic pathways to detoxify oxygen radicals.
Pathogenic microorganisms similarly have unique niches that they favor when they colonize the human body. Due to their inability to tolerate oxygen, obligate anaerobic pathogens such as C. difficile are primary gastrointestinal pathogens, growing where oxygen concentrations are low or absent [1]. In contrast, facultative anaerobes (i.e., bacteria that can grow in both oxygenated and anoxic environment) such as S. aureus can colonize and infect a variety of different locations on and in the body [2], ranging from skin to deep-tissue infections.
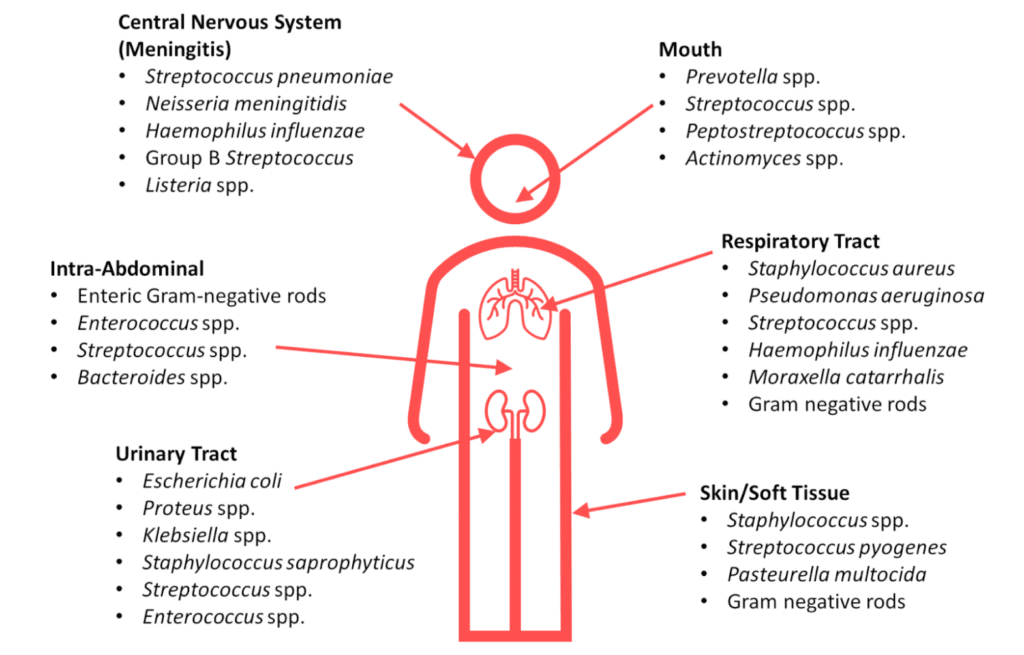
Due to these metabolic requirements, there is often a predictable set of microorganisms that commonly cause infections in specific parts of the body.
Below is a figure of some of the common bacteria for select site of infection.
In addition to choosing a pathogen that’s appropriate for a location on the body, another important consideration is choosing a relevant antibiotic for use as a control or comparator. Antibiotic penetration in the body is dependent on their hydrophilicity or lipophilicity, with the former having lower intracellular penetration and the latter having higher intracellular penetration. As such, hydrophilic antibiotics are rarely used to treat intracellular infections, such as Shigella and Listeria [4].
In addition, antibiotics are broadly classified as broad spectrum or narrow spectrum. Broad spectrum antibiotics are active against a wide range of different bacteria, e.g., Ampicillin, which is active against Gram-positive and Gram-negative species. Narrow spectrum antibiotics are active against a select group of microbes, e.g., Fidaxomicin, which is used to treat C. difficle gastrointestinal infections.
In a clinical setting, broad spectrum antibiotics are often the first line of treatment even before the infectious organism is identified. The selection of the antibiotic is often based on the location of the infection on the patient (see figure above) as well as the local antibiotic resistance pattern monitored by regional public health authorities.
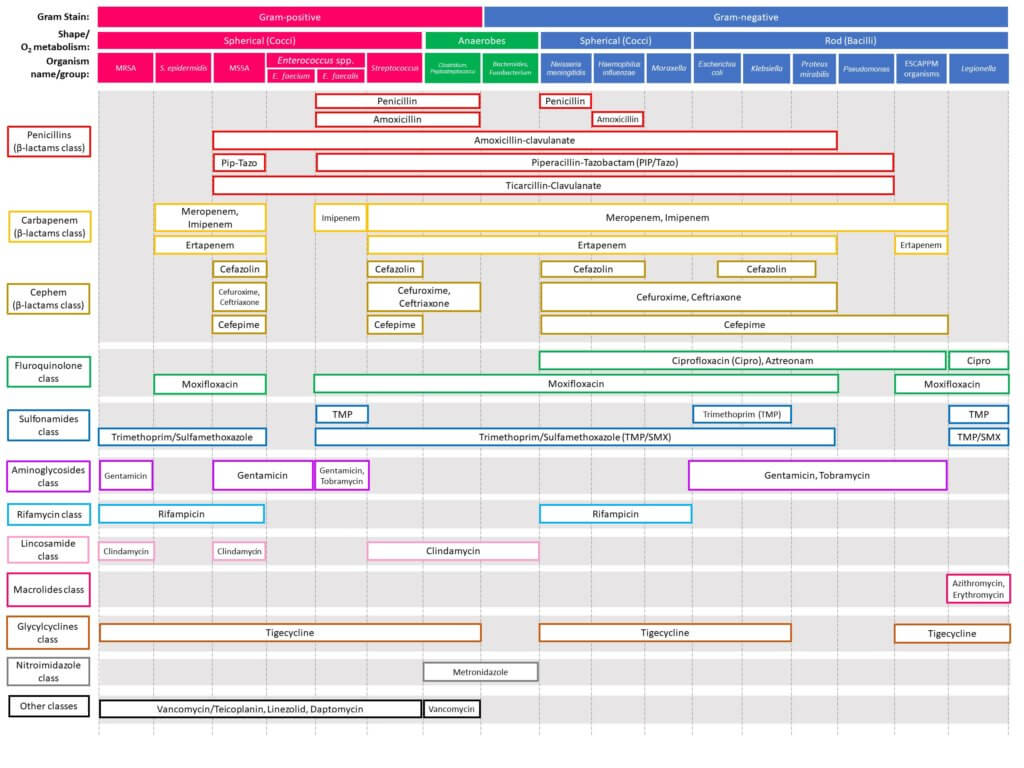
The figure below shows a simplified view of general antibiotic coverage.
If a novel compound being developed is based on an existing antibiotic, then the most appropriate control would be the parent molecule that the new drug is derived from. If the drug under development has no chemical or structural similarities to known antibiotics, then a suitable comparator would be an existing antibiotic that’s commonly used to treat the relevant infection.
That being said, one of the first questions that innovators ask themselves when they synthesize a new compound is “what is this active against?” In situations like that, Emery Pharma has developed screening panels that can help guide the drug development process. Combined with our years of regulatory experience, we can help you not only choose the right tools to use in testing your new drug, but also help to bring it to market.
Citations
- Kint N, Alves Feliciano C, Martins MC, Morvan C, Fernandes SF, Folgosa F, Dupuy B, Texeira M, Martin-Verstraete I. How the Anaerobic Enteropathogen Clostridioides difficile Tolerates Low O2 mBio. 2020 Sep 8;11(5):e01559-20. doi: 10.1128/mBio.01559-20.
- https://www.canada.ca/en/public-health/services/laboratory-biosafety-biosecurity/pathogen-safety-data-sheets-risk-assessment/staphylococcus-aureus.html
- Rachitskaya AV, Flynn HW, Davis JL. Endogenous Endophthalmitis Caused by Salmonella Serotype B in an Immunocompetent 12-Year-Old Child. JAMA Ophthalmology. 2012;130(6):802–804. doi:10.1001/archophthalmol.2011.1862
- Catania R, Mastrotto F, Moore CJ, Bosquillon C, Falcone FH, Huett A, Mantovani G, Stolnik S. Study on Significance of Receptor Targeting in Killing of Intracellular Bacteria with Membrane-Impermeable Antibiotics. Advanced Therapeutics. 2021;4(12). Doi: 10.1002/adtp.202100168